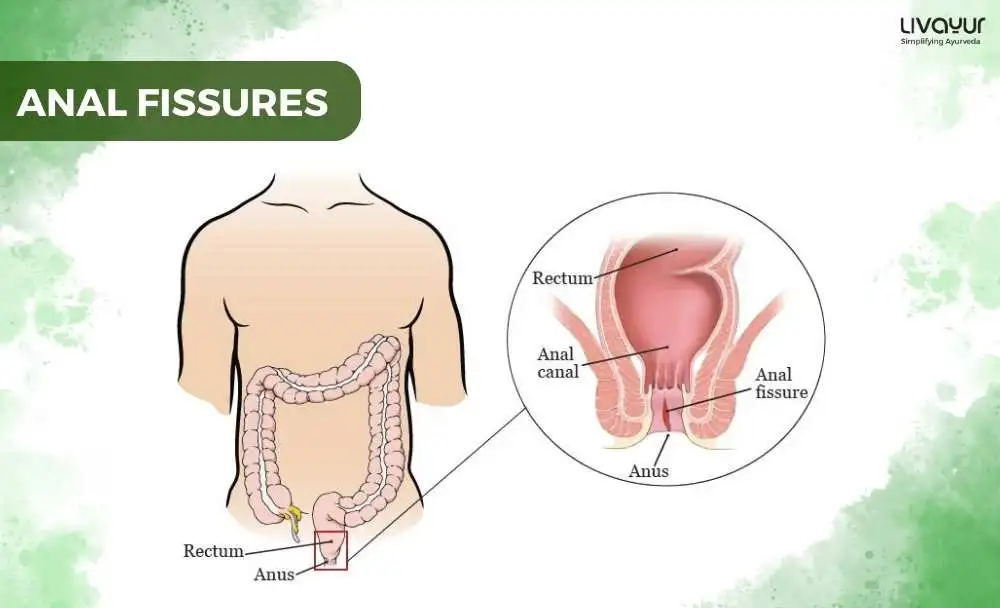
An anal fissure is a common medical condition that affects the anus and can cause significant discomfort and pain. It is characterized by a tear or ulceration in the epithelial lining of the anal canal, which can cause pain, bleeding, and itching. [1]
Anal fissures can be acute or chronic and are often associated with conditions such as constipation, diarrhea, or inflammatory bowel disease. In this article, we will discuss the anal fissure causes, the anal fissure symptoms and treatment, the anal fissure prevention tips, Ayurvedic management of anal fissures, home remedies for anal fissures and much more. Read on:
Anal fissure symptoms
Symptoms of anal fissures can vary depending on the severity of the condition, but the most common symptoms include:
1. Pain during bowel movements
Anal fissures can cause sharp, severe pain during bowel movements that may last for several hours. The pain is usually described as burning, tearing, or stinging, and it can be so intense that it causes the person to avoid going to the bathroom. [1]
2. Bleeding
A small amount of bright red blood may be seen on the toilet paper or in the toilet bowl after a bowel movement. This occurs because the anus has torn and the blood vessels in the area have been damaged. [1]
3. Itching or irritation
The skin around the anus may become irritated and itchy as a result of the fissure. [13]
4. Muscle spasms
Some people may experience involuntary muscle spasms in the anal area, which can worsen pain and discomfort. [2]
It is important to note that these symptoms can also be indicative of other conditions such as hemorrhoids or inflammatory bowel disease, so it is important to seek medical attention for proper diagnosis and treatment.
Causes of anal fissure
Anal fissures can be caused by a variety of factors listed below:
1. Constipation
Constipation can cause hard stools that stretch the anal canal and lead to tearing and formation of fissures. [2]
2. Diarrhea
Chronic diarrhea may irritate the anal area and lead to the formation of fissures. [13]
3. Trauma to the anal canal
Trauma to the anal area can occur during childbirth or from anal sex which may eventually lead to the formation of fissures. [3]
4. Inflammatory bowel disease
Inflammatory bowel disease, such as Crohn’s disease or ulcerative colitis, can also increase the risk of anal fissures. [6]
Treatment for Anal Fissure
Treatment options for anal fissures include both non-surgical and surgical interventions.
Non-surgical treatment options include:
1. Topical Medications
Over-the-counter creams and ointments such as hydrocortisone for anal fissures and lidocaine for anal fissures can help to reduce pain and inflammation in the affected area. Prescription-strength medications may also be prescribed by a healthcare provider. [1]
2. Stool Softeners
Hard stools can exacerbate anal fissures and make them more painful. Taking stool softeners such as docusate sodium can help to make bowel movements less painful and reduce the risk of further injury. [2]
3. Dietary Changes
Increasing fiber intake and drinking plenty of water can help to soften stools and reduce constipation, which can, in turn, reduce the risk of anal fissures. It is also important to avoid spicy and acidic foods, which can irritate the anal area. [2]
4. Sitz Baths
Soaking in warm water for 10-15 minutes several times per day can help to soothe the anal area and promote healing. Adding Epsom salts or other soothing agents to the water can also be beneficial. [2] [4]
Surgical treatment options include:
If non-surgical interventions are not effective, surgery may be necessary. The two main surgical options for anal fissures are:
1. Lateral Internal Sphincterotomy
This procedure involves cutting the muscle that controls the anus, which can reduce pressure on the fissure and promote healing. It is typically done under general anesthesia and requires a short hospital stay. [1]
2. Anal Fissurectomy
This procedure involves surgically removing the scarred tissues and damaged superficial skin around the fissure. Aged patients with an issue of incontinence or multiparous female patients or patients who have undergone anorectal surgery in the past are generally treated with this surgical procedure. [14]
It is important to note that the choice of treatment will depend on the severity of the fissure, as well as the individual’s overall health and medical history. A healthcare provider can help to determine the most appropriate treatment plan.
Ayurvedic treatment & home remedies for anal fissures
Ayurveda offers various remedies for anal fissures, aiming to alleviate discomfort and promote healing. Also, there are some age-old home remedies to help you deal with the pain and discomfort associated with anal fissures. Here are some treatments and remedies commonly used:
1. Avgaha Sweda (Sitz Bath):
This involves sitting in a warm bath with added medicinal herbs like Triphala (a combination of three fruits) or Neem. It helps soothe the area, reduce inflammation, and promote healing. [10]
2. Jatyadi Ghee/Oil:
Jatyadi oil is an Ayurvedic preparation containing ingredients like Jatiphaladi, Manjistha, and Turmeric(Haridra) in a base of sesame oil or ghee. It is applied topically to the affected area to reduce inflammation and aid in healing. It helps in reducing itching, burning, and irritation while acting as an antibacterial agent. In severe cases where it might be combined with Rajat Bhasma and Gandhak Rasayana for enhanced effectiveness. [7]
3. Triphala Guggulu:
Triphala Guggulu aids in preventing constipation and easing stool passage, a primary factor in anal fissures. It also possesses analgesic properties and can be substituted with Gulkand or Triphala Churna for mild constipation cases. [7]
4. Yashtimadhu Ghrita:
This Ayurvedic formulation comes with anti-ulcerogenic and anti-inflammatory properties and helps in skin regeneration too. Therefore, it proves to be highly effective in healing anal fissures. [9]
5. Gandhak Rasayana:
This drug plays a crucial role in preventing infections and itching and in promoting the healing of fissures. [10]
6. Haridra or Turmeric:
With its antimicrobial and anti-inflammatory characteristics, turmeric safeguards against secondary infections, curbs bleeding in hemorrhoids, and alleviates anal itching. [10] [11]
7. Kshar Sutra Treatment:
In chronic stages, therapies involving Kshar Sutra ligation followed by Kshar Karma are employed to eliminate the fissure. [8]
8. Yoga Prana Vidya Healing:
Yoga Prana Vidya treatment protocol for anal fissure has yielded results in managing the issue in patients who had been suffering from anal fissures for several years. This healing protocol makes use of the Prana or life force to treat health issues at a physical as well as psychological level. [12]
9. Petroleum Jelly:
Applying petroleum jelly around the anal region aids in soothing the skin, serving as an home remedy for anal fissures. It can be applied multiple times a day for relief.
10. Hydration:
Adequate water intake, about six to eight glasses daily, prevents dehydration and softens stool, easing constipation. Increased hydration helps relieve pressure, subsequently alleviating pain and muscle spasms around the anal region. [6]
11. Dietary Fiber:
Boosting daily fiber intake through fruits, vegetables, whole grains, and legumes aids in softening stool, addressing constipation, and reducing pressure. Adults should aim for around 18 grams of fiber daily. [2] Examples of high-fiber foods include:
- Vegetables and fruits
- Legumes like peas, lentils, and beans
- Soy-based products and soy milk
- Flaxseed, oat brans, barley, psyllium, and seed husks
- Nuts and seeds
- Whole-grain foods
How to avoid anal fissure?
You can avoid anal fissures by following the given steps:
1. Reversing constipation [2]
You need to maintain healthy bowel habits and treat your constipation in the first place. Constipation may be managed by eating a high-fibre diet, drinking plenty of water, and exercising regularly.
2. Using stool softeners
Hard stool may cause straining during bowel movements, and that increases the risk of anal fissures. Using a stool softener or fibre supplement can help you avoid straining. [5]
3. Avoiding trauma to the anal area
Avoiding trauma to the anal area, such as from anal sex or childbirth, is also important for anal fissure prevention. [6]
FAQs
1. Is an anal fissure considered a serious issue?
An anal fissure, characterized by a tear in the lining of the lower rectum, often causes discomfort during bowel movements. Generally, anal fissures are not considered serious issues and typically heal with home treatments within a few days or weeks. These are commonly termed as short-term or acute anal fissures and do not usually progress to more severe complications.
2. Can anal fissure be taken care of at home?
Yes, a number of anal fissures can heal with proper self-care measures, particularly if one can avoid constipation. Taking a Sitz bath for about 20 minutes, two to three times daily, is recommended as part of home care. This can be done in a bathtub or using a specialized Sitz bath kit. With diligent self-care and efforts to prevent constipation, some anal fissures have the potential to heal naturally without additional intervention.
3. Does walking aggravate anal fissure?
Walking, in fact, contributes to overall health and can be beneficial if you have an anal fissure. It can reduce the likelihood of developing hard stools and supports improved blood circulation, which can be helpful in managing a fissure.
4. How do fissures, piles, and fistulas differ in terms of symptoms and severity?
Piles primarily involve swollen blood vessels, whereas fissures manifest as cracks, and fistulas are characterized by cavity openings. While piles may often be painless and inconspicuous, fissures usually induce significant pain. In cases of fistulas, discharge of pus occurs in the anal area.
5. What are effective topical treatments for fissures?
Petroleum jelly, zinc oxide, 1% hydrocortisone cream, and options like Preparation H are beneficial for soothing the affected area. Opt for alcohol-free baby wipes instead of harsh toilet paper for gentler cleansing. Incorporating Sitz baths into your routine can aid in fissure healing and provide relief.
Conclusion
In conclusion, anal fissures are a common medical condition that can cause significant discomfort and pain. They are often associated with conditions such as constipation, diarrhoea, or inflammatory bowel disease. Treatment options include over-the-counter creams and ointments, prescription medications, and surgery. Prevention involves maintaining healthy bowel habits and avoiding trauma to the anal area. With proper treatment and prevention, most cases of anal fissures can be successfully managed.
Disclaimer:
The information provided in this article is for education and general awareness. It is not intended to substitute any medical advice. Please consult your healthcare professional for any medical information.
References:
- Anal Fissure
- Anal Fissure
- Benign Anorectal: Anal Fissure
- The effect of salty warm sitz bath on the conservative management of anal fissure
- Anal Fissure
- Anal fissure: diagnosis, management, and referral in primary care
- Clinical evaluation of ayurvedic compound and manual dilatation of anus in the management of parikartika (fissure-in ano): An open perspective study
- A Clinical Study on Chronic Anal Fissure by ligating Ksharasutra (medicated thread) w.s.r. to Sphincterotomy
- A comparative clinical study of Yashtimadhu Ghrita and lignocaine-nifedipine ointment in the management of Parikartika (acute fissure-in-ano)
- PARIKARTIKA: FISSURE IN ANO
- Comparative study of Ksharasutra suturing and Lord’s anal dilatation in the management of Parikartika (chronic fissure-in-ano)
- Anal Fissures: A Case Series Study On How Yoga Prana Vidya (YPV) HealingProtocols Treated This Condition And Associated Symptoms
- Anal Fissure- A Common Cause of Anal Pain
- Fissurectomy Versus Lateral Internal Sphincterotomy in the Treatment of Chronic Anal Fissure- A Randomized Control Trial