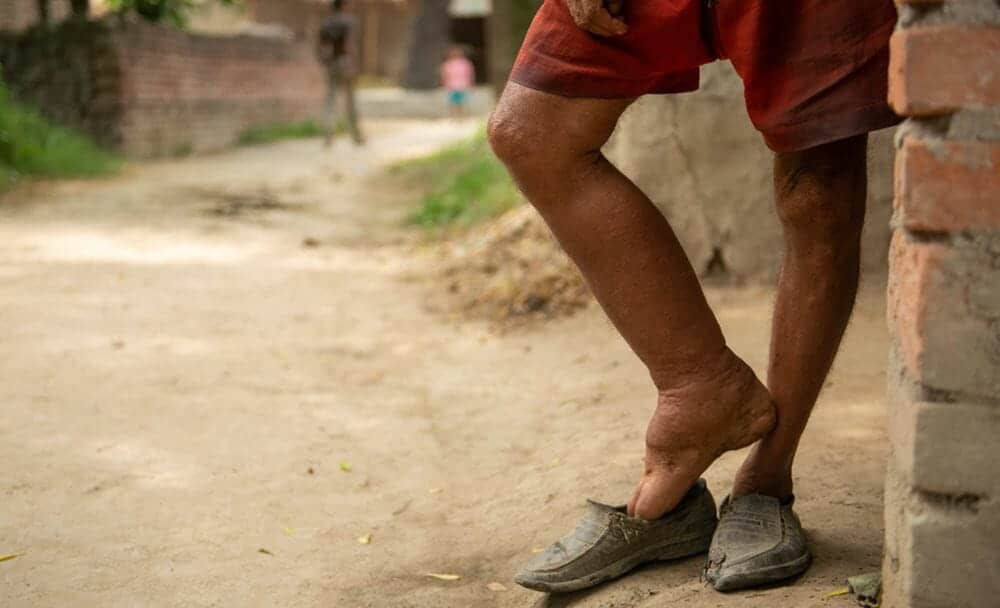
Elephantiasis, also known as lymphatic filariasis, is a debilitating and disfiguring condition that primarily affects the lymphatic system, leading to the enlargement of body parts, particularly the limbs, breasts, or genitals. Parasitic worms cause this disease and can have severe physical and psychological impacts on those affected. [1]
Concerning the origin of Shlipada according to Vagbhata, he explains that the bodily humors or Doshas, primarily Kapha, gather in the lower part of the body over time, particularly in the inguinal region and thigh, using the feet as a foundation. This accumulation results in the development of a thick swelling known as “Sopham,” which is termed as Shlipada or elephant disease. [3]
This comprehensive article will delve into the symptoms, the elephant foot disease caused by what, and the treatment of elephant leg disease in individuals.
Symptoms of Elephantiasis
Some common elephant leg disease symptoms include:
Swelling:
The most recognizable symptom of elephant foot disease is swelling in the affected body part, often leading to extreme enlargement. This is most commonly observed in the limbs and genitals. [1]
Pain and Discomfort:
The swelling can cause pain, discomfort, and heaviness, making it difficult for individuals to move and carry out daily activities. [2]
Thickened Skin:
The skin over the swollen area becomes thick and rough and can develop a nodular appearance. [2]
Skin eruptions:
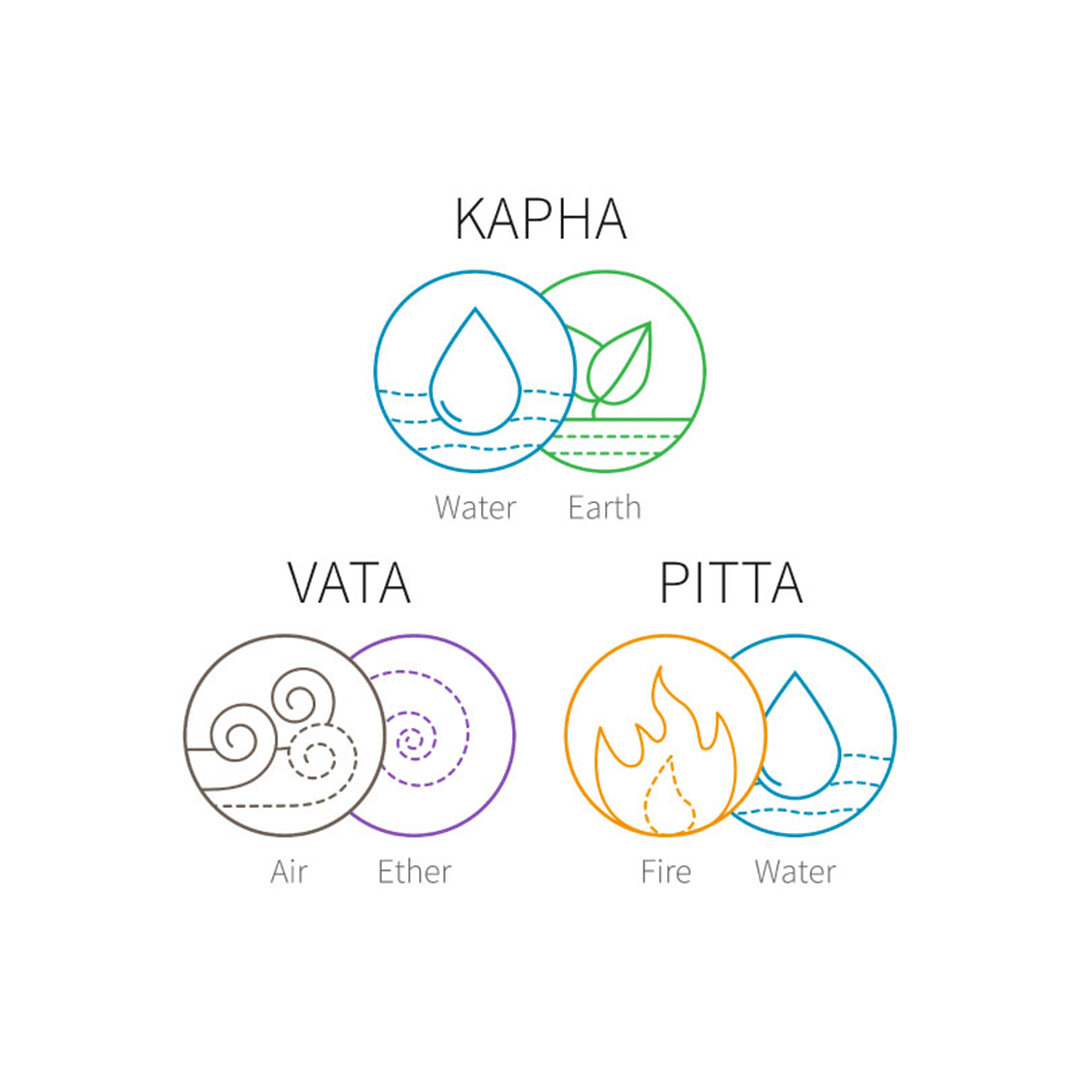
Shlipada arises due to Vata Dosha, elephant disease is characterized by small eruptions, dark color, unexplained pain, rough texture, and dry appearance. [3]
Fever:
If elephant disease is caused by Pitta Dosha, it appears yellow with a burning sensation and fever. [3]
Nodes on skin:
Shlipada or elephant disease originating from Kapha dosha is large, heavy, unctuous, devoid of pain, and surrounded by fleshy nodes. [3]
Other symptoms:
Elephant disease can have a significant effect on the immune system leading to restrictive pulmonary lung disease, wheezing, shortness of breath, and eosinophilia. [2]
Causes of Elephantiasis
Elephant foot disease caused by infection with parasitic worms, specifically Wuchereria bancrofti, Brugia malayi, and Brugia timori occurs due to unhygienic living conditions. These worms are transmitted to the human body through the bites of infected mosquitoes, primarily from the genera Culex, Anopheles, Mansonia, Ochlerotatus, and Aedes. When an infected mosquito bites a person, it transfers the microscopic larvae of the parasitic worms into their bloodstream.
Once inside the body, these larvae mature into adult worms in the lymphatic vessels. The females release numerous microfilariae into circulation daily for about five years and up to 9 years.
As adult worm numbers increase, they block the lymphatic system, disrupting drainage and making the body more susceptible to recurrent infections. Elephant leg disease caused by this ongoing inflammation, a mix of acute and chronic, triggers lymphatic tissue scarring and restructuring, contributing to the visible skin changes characteristic of elephantiasis. [2]
Treatment of elephantiasis
The elephant leg disease treatment focuses on relieving symptoms, managing complications, and preventing further disease progression. Common treatment approaches include:
Ayurvedic management:
Venesection:
For all types of Shlipada, this is recommended. In the case of Vatika-type Shlipada, the vein about two finger-widths above the ankle is incised after treating it with Upanaha as a preparatory step. [3]
Decoctions:
Concoctions infused with honey and gradually escalating doses of Haritaki (Chebulic myrobalan) should be consumed. [3]
Lepas:
Mustard, eggplant, or coriander can be employed for external applications as Lepas. Apart from this, a mixture of finely powdered Nonganampullu and turmeric and a handful of uncooked rice, boiled in the strained water from washing rice, is prepared. This concoction is applied to the affected area, which is then covered with a leaf from the Clerodendrum viscosum plant to alleviate elephant disease symptoms effectively. [3]
Black pepper:

Incorporating black pepper into the daily diet or beverages aids in the prevention of filariasis or elephant disease. [3]
Non Ayurvedic management:
Medication:

Antiparasitic medications, such as diethylcarbamazine (DEC) or ivermectin, are prescribed to kill adult worms and larvae. [2]
Management of Complications:
Treating infections, addressing skin-related issues, and managing pain are essential to improve the quality of life for individuals with elephant disease. [2]
Elevation and Compression:
Elevating the affected limb and using compression bandages or garments can help reduce swelling and improve lymphatic flow. [2]
Surgery:
In severe cases where conservative treatments fail, surgical procedures may be considered to debulk skin and improve drainage.[2]
FAQs
• How can elephantiasis be diagnosed?
Diagnosing elephantiasis involves peripheral smear, PCR, or scrotal ultrasound.
1. Peripheral Blood Smear Preparation: There are two thick and thin peripheral blood smear samples created which can be obtained through venipuncture or finger/heel stick methods. These samples are usually collected after 8 pm due to the nightly presence of microfilariae.
2. PCR for Antigen Detection: Polymerase Chain Reaction (PCR) is employed for identifying antigens. This technique is favored for diagnosis as it can also identify dormant infections.
3. Scrotal Ultrasound: Scrotal ultrasound has the potential to uncover the movement of adult worms in males without evident symptoms. The “filarial dance sign” refers to a distinctive pattern of worm movement observed in infected men’s lymphatic vessels during such ultrasound examinations. [2]
• How can elephantiasis be prevented?
Preventing elephant disease requires a multifaceted approach:
1. Controlling mosquito populations through bed nets, insecticides, and environmental management can help prevent the spread of the disease.
2. In endemic areas, Mass Drug Administration campaigns involve distributing anti-parasitic medications to the entire population to target the transmission of the disease.
3. Raising awareness about elephantiasis causes, transmission, and prevention is crucial for encouraging individuals to take preventive measures.
4. Improving one’s access to clean water and proper sanitation facilities can reduce the breeding sites for mosquitoes and limit exposure to parasites.
• Who is susceptible to elephantiasis?
Frequent risk factors associated with elephant skin disease encompass residing in tropical and subtropical regions for extended periods, increased exposure to mosquitoes, and living in unhygienic environments.
Conclusion:
Elephant disease is a complex and debilitating disease affecting millions worldwide, primarily in tropical and subtropical regions. The physical, psychological, and economic burdens it places on individuals and communities are significant. Efforts to control and prevent elephant leg disease causes require medical treatment, vector control, education, and improved infrastructure. By addressing the root causes of this disease and implementing effective prevention measures, we can work towards reducing the prevalence of elephantiasis and alleviating its impact on those who suffer from it.
Disclaimer:
This article is written from a health and wellness perspective and is not medical advice. Kindly seek the help of a certified medical practitioner before initiating any treatment.
References: