Reviewed By Dr. Vipin Bihari Sharma
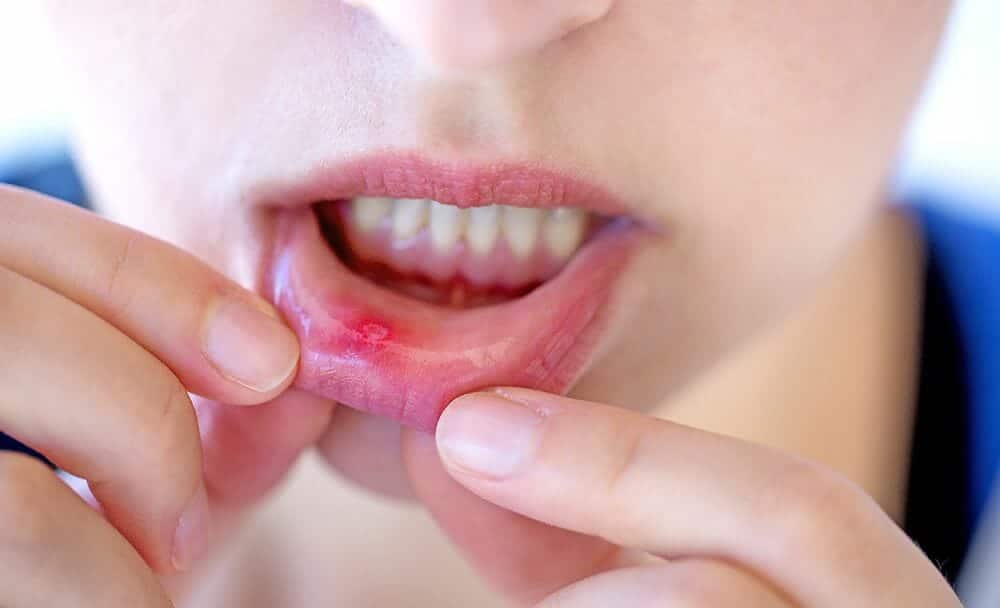
Stomatitis is a general term that refers to mucous membrane inflammation inside your mouth. It can occur in people of all ages but is more common in women than in men. Stomatitis can be of various types and can occur due to various factors such as Candida infections, denture trauma, nighttime denture wearing, denture cleanliness, dietary factors, and predisposing systemic conditions. It can cause pain, discomfort, and swelling, making it difficult to eat, drink, and speak properly. [1] Stomatitis meaning in Hindi is mouth ulcers, and these are a commonly occurring oral condition, often influenced by improper food habits and lifestyle choices. Among the various factors contributing to their development, Apathyakara ahara (improper food habits) and vihara (lifestyle) play significant roles. [8]
In this article, we will explore stomatitis in detail, including its causes, symptoms, types, prevention, and treatment options.
Causes of Stomatitis:
There are various stomatitis causes, including:
Viral Infections:
Many cases of Aphthous stomatitis are triggered by viral infections like the one caused by herpes simplex virus (HSV). [3]
Bacterial Infections:
Certain bacteria, due to poor dental or oral hygiene, high carbohydrate intake, and reduced salivary flow, can cause denture stomatitis, particularly when there is a breach in the oral mucosa. [1]
Fungal Infections:
Candida albicans, a type of yeast inhabiting the dental surface where they adhere very well, can cause oral thrush, leading to stomatitis. These microorganisms develop in areas from where they are not easily removed by mechanical or chemical cleansing. [1]
Allergic Reactions:
Some people may develop stomatitis as a result of an allergic reaction to certain oral products, such as constituents of the denture material. This could be due to the presence of resin monomer, dimethyl-p-toluidine, hydroquinone peroxide, or methacrylate in the denture. [1] Aphthous stomatitis could also occur due to sensitivity to sodium lauryl sulfate present in toothpaste and oral hygiene products, foods such as cinnamon, cheese, citrus, figs, or pineapple. [3]
Nutritional Deficiencies:
Deficiencies in iron, folate or vitamin B12, or other nutrients can lead to stomatitis. [1]
Trauma:
One of the main causes of denture stomatitis is trauma which can be in the form of denture trauma due to ill-fitting dentures or nocturnal wear of dentures. [1]
Other factors:
Other factors like hypothyroidism, weakened immune system conditions (such as HIV infection), certain cancers (such as acute leukemia and agranulocytosis), and the use of immune-suppressing medications (like corticosteroids) can increase the susceptibility of individuals to develop candida-associated denture stomatitis. [1]
Symptoms of Stomatitis:
Stomatitis symptoms can vary depending on the underlying cause, but common signs and symptoms may include:
- A burning discomfort a couple of days prior to the onset of ulcerations
- Pain or discomfort in common locations such as the buccal (cheek) and labial (lip) mucosa, the mouth’s floor, the tongue’s underside, and the soft palate.
- Inflammation of the oral mucosa, which may be oval or round in shape and vary in its size from nearly 1 to 3 cm in diameter.
- Aphthous stomatitis ulcers are characterized by well-defined sores or ulcers in the mouth, which may be white or yellowish and surrounded by a red border. [3]
- Difficulty speaking, eating, drinking, or swallowing.
- Fever, headache, cough, and general malaise can also be stomatitis symptoms in some cases. [4]
Types of Stomatitis:
Stomatitis can manifest in different forms, including:
Herpetic Stomatitis:
Caused by the herpes simplex virus, herpetic stomatitis [5] is characterized by painful cold sores or blisters on the lips, tongue, gums, or inside cheeks, especially in young children. [6]
Aphthous Stomatitis:
Also known as canker sores, aphthous stomatitis is a common type of stomatitis characterized by small, shallow ulcers that appear on the inner cheeks, lips, tongue, or throat. These ulcers can be painful and may recur. [3]
Angular Stomatitis:
Angular stomatitis, or angular cheilitis, is characterized by the presence of cracks, redness, and lesions on the lips. It is often associated with a viral or bacterial infection. [7]
Prevention of Stomatitis:
Although not all cases of stomatitis can be prevented, some measures can help reduce the risk of developing this condition:
Good Oral Hygiene:

Brushing and flossing at least two times a day can help maintain oral health and prevent infections. [1]
Prevent trauma:
Implant overdentures have the potential to effectively manage denture stomatitis by reducing trauma to the oral mucosa in elderly individuals without teeth. You can get improved oral mucosal health in the upper jaw when lower dentures are supported by at least two implants. [1]
Quit smoking and control sugar intake:
Refrain from smoking and high intake of sugary substances in your diet. If you consume a high amount of sugar, it is important to note that glucose promotes the growth of Candida and its adherence to the surface of the dentures. [2]
Maintaining a Balanced Diet:
A well-balanced diet rich in essential vitamins and appropriate carbohydrate intake can support oral health and help prevent nutritional deficiencies that may contribute to stomatitis. [2]
Avoiding Triggering Factors:
If you have a known allergy or sensitivity to certain foods, medications, or oral care products, avoiding them can help prevent stomatitis. [3]
Stress Management:
Managing emotional or physiologic stress levels through relaxation techniques or counseling can help prevent stress-induced stomatitis in some individuals. [3]
Recent findings:
Recent studies have shown that you can prevent stomatitis by applying protective coatings on the denture surface to minimize Candida adhesion, incorporating antibodies that specifically target Candida species into the material of the prosthesis, and utilizing antifungal agents within the denture material to inhibit Candida growth. [2]
Treatment of Stomatitis:
The treatment of stomatitis depends on the underlying cause and the severity of symptoms. Here are some common treatment options:
Ayurvedic treatment:
Gandush:
One topical stomatitis treatment option is the use of Gandush, which involves rinsing the mouth with a concentrated solution of Darvi (a medicinal plant) mixed with honey. This practice exerts a direct effect on the oral mucosa by creating increased mechanical pressure within the oral cavity. The active constituents present in Gandush stimulate the parasympathetic fibers of the salivary gland, leading to abundant saliva secretion.
Saliva contains immunoglobulin Ig, which possesses antimicrobial and antiviral properties, contributing to the management of mouth ulcers.
Darvi:
Also known as Daruharidra, this is a medicinal herb widely recognized for its antibacterial, antipyretic, anti-inflammatory, and analgesic properties. When combined with Madhu (honey), Daruharidra becomes beneficial in the treatment of conditions such as aphthous stomatitis.
The Kashya rasa (astringent taste) of Daruharidra aids in wound healing and helps alleviate imbalances related to Kapha, Rakta, and Pitta doshas.
Honey, known for its cooling properties, helps reduce bleeding disorders and balances Kapha, while also promoting wound healing. It also provides clarity in the oral cavity, aids in the healing of ulcers, and alleviates burning sensations. [8]
Medications:
Antifungal therapy may be prescribed as stomatitis treatment, depending on the cause of stomatitis as these mechanisms function by impeding the processes (such as enzymes, substrates, and transport) required for the synthesis of the fungal cell membrane. [1]
Topical Treatments:

Topical gels, mouthwashes, or topical agents such as amphotericin B lotion and Nystatin can provide relief and promote the healing of oral ulcers and act as an effective stomatitis treatment. [1]
Antiseptics:
Disinfecting agents like sodium hypochlorite and chlorhexidine are utilized to eradicate denture plaque and prevent candida colonization on the surface of the denture. [1]
Oral Care Practices:
Maintaining good oral hygiene and gently cleaning the mouth and plaque control by careful brushing and overnight denture soaking in 0.1% aqueous chlorhexidine can promote healing and prevent secondary infections. [1]
Surgical intervention:
While for mild cases of inflammatory papillary hyperplasia or low stomatal index, non-surgical antifungal treatment can be considered, in severe cases, cryosurgery or excision may be considered for the treatment of palate papillary hyperplasia. [1]
Dietary supplementations:
Dietary supplementations may be recommended for individuals deficient in iron, zinc, or vitamins B1, B2, B6, B12, or C. [3]
FAQs
1. How can stomatitis be cured fast?
While there is no instant cure for stomatitis, certain measures can help speed up the healing process. These include practicing good oral hygiene, using topical treatments prescribed by a healthcare professional, avoiding irritants, maintaining a balanced diet, and managing underlying conditions that may contribute to stomatitis.
2. How serious is stomatitis?
The seriousness of stomatitis varies depending on the underlying cause, severity of symptoms, and individual factors. In most cases, stomatitis is a temporary and relatively mild condition. However, severe cases of stomatitis, especially when associated with systemic infections or underlying medical conditions, may require medical intervention and management.
3. What foods can cause stomatitis?
Trigger foods for stomatitis include spicy foods, acidic fruits, rough or crunchy foods, allergenic foods (e.g., nuts, shellfish), and irritating additives.
Conclusion:
Stomatitis is a common condition characterized by inflammation and ulcers in the mouth. It can be caused by various factors, including viral or bacterial infections, allergies, nutritional deficiencies, trauma, or autoimmune disorders. The symptoms and types of stomatitis can vary, but they often involve pain, ulcers, and difficulty eating. Preventive measures such as good oral hygiene, avoiding irritants, and maintaining a balanced diet can help reduce the risk of stomatitis. Treatment options include medications, topical treatments, pain relief, oral care practices, dietary modifications, and managing underlying conditions.
Disclaimer:
This article is written from a health and wellness perspective only and is not a piece of medical advice. Kindly seek the help of a certified medical practitioner before initiating any treatment.
References:
- Denture Stomatitis: A Literature Review
- DENTURE STOMATITIS – A REVIEW
- Aphthous Stomatitis
- Recurrent Aphthous Stomatitis: A Review
- Stomatitis, Herpetic
- Herpetic Gingivostomatitis
- Down syndrome: Lip lesions (angular stomatitis and fissures) and Candida albicans
- Ayurvedic Management of Mukhapaka w. s. r. To Stomatitis : A case Study