Malnutrition is a serious global health issue that affects millions of individuals, particularly children, in developing countries. Two common forms of malnutrition are Kwashiorkor and Marasmus also known as Parigarbhika and Balshohsa respectively in Ayurveda. [1] Although both conditions result from insufficient nutrient intake, they have distinct characteristics and require different approaches for treatment. In this article, we will explore the differences between Kwashiorkor and Marasmus, including their causes, symptoms, and management strategies.
Understanding Kwashiorkor
Kwashiorkor is a form of severe protein-energy malnutrition characterized by inadequate protein intake while consuming enough calories overall. This condition often occurs in children aged 1 to 3 years who have recently weaned off breast milk and transitioned to a diet lacking in protein-rich foods. The name “Kwashiorkor” originates from the Ga language of Ghana, meaning “the sickness the older child gets when the new baby comes.” [2]
Causes of Kwashiorkor
Although the exact cause of Kwashiorkor is still being researched, the most widely accepted hypothesis is that the primary cause of Kwashiorkor is a diet deficient in protein. This can happen due to various factors, including insufficient food intake with Inadequate consumption of protein-rich foods and dairy products. Limited access to nutritious food due to poverty, food insecurity, and lack of resources can also restrict access to a diverse and balanced diet. In many cases, underlying infections, such as gastrointestinal infections or parasites, can hinder nutrient absorption and increase protein requirements which eventually leads to the patient becoming malnourished. [3] [4]
Symptoms of Kwashiorkor
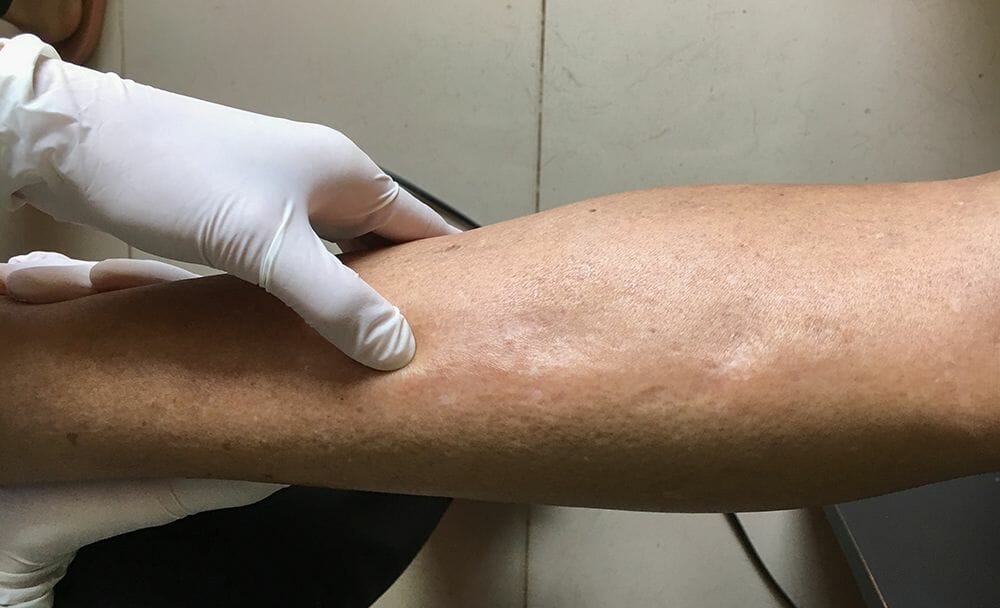
Children with Kwashiorkor often exhibit several distinctive symptoms, including:
- Edema: Swelling of the feet, ankles, and legs due to fluid accumulation. [5] [6]
- Skin and hair changes: Dry, thin, and flaky skin, along with hair that is brittle and easily plucked. [5] [6]
- Fatty liver: Enlargement of the liver due to excessive accumulation of fat. [5] [6]
- Stunted growth: Impaired physical and cognitive development due to nutrient deficiencies. [5] [6]
- Loss of appetite: Children may have a reduced desire to eat or experience taste changes. [5] [6]
Management of Kwashiorkor

The treatment of Kwashiorkor involves a multidimensional approach, including:
- Nutritional rehabilitation: Providing a balanced diet that is rich in high-quality protein, essential vitamins, and minerals. This may involve therapeutic feeding programs, fortified foods, and nutritional supplements. [5] [6]
- Medical intervention: Addressing any underlying infections or diseases that may be contributing to the condition. [5] [6]
- Supportive care: Monitoring and managing complications such as edema, electrolyte imbalances, and infections. [5] [6]
- Education and counseling: Educating caregivers about proper nutrition, hygiene practices, and long-term prevention of malnutrition. [5] [6]
Understanding Marasmus
The name “Marasmus” originates from the Greek word marasmos(withering) which loosely translates to “wasting away”. It is another form of severe malnutrition that primarily results from a deficiency in both calories and protein. Unlike Kwashiorkor, Marasmus typically occurs in infants who are less than a year old.
Causes of Marasmus
The main causes of Marasmus include an insufficient consumption of calories and protein due to poverty, famine, or inadequate feeding practices. Infants born to malnourished mothers and especially mothers suffering from illnesses like HIV are at higher risk of developing Marasmus. Most importantly premature introduction of solid foods without proper nutritional value leads to inadequate nutrient intake. [7] [8] [9] [10]
Symptoms of Marasmus
Children with Marasmus exhibit severe overall malnutrition and present with the following symptoms:
- Severe weight loss: Children experience significant muscle wasting and become emaciated. [7] [8]
- Growth retardation: The child’s growth is stunted, both physically and mentally. [7] [8]
- Weakness and lethargy: Due to energy deprivation, children may appear weak, tired, and lack energy. [7] [8]
- Loss of subcutaneous fat: The absence of fat under the skin results in a gaunt appearance. [7] [8]
- Impaired immune function: Malnutrition weakens the immune system, making the child susceptible to infections. [7] [8]
Management of Marasmus
The treatment of Marasmus focuses on gradual nutritional rehabilitation and addressing underlying health issues. The management strategies for Marasmus include:
- Nutritional rehabilitation: Providing a carefully calculated and gradually increased caloric intake, starting with easy-to-digest foods such as fortified milk, followed by a gradual introduction of solid foods. [7] [8]
- Close monitoring: Regular weighing and assessing the child’s growth, nutritional status, and any complications that may arise. [7] [8]
- Hydration management: Ensuring adequate fluid intake to address electrolyte imbalances and dehydration. [7] [8]
- Emotional support: Providing emotional support to caregivers and educating them about proper feeding practices, hygiene, and the importance of continued follow-up care. [7] [8]
What’s the difference between Kwashiorkor and Marasmus?
Kwashiorkor and Marasmus are both severe forms of malnutrition, but they differ in their underlying causes and clinical characteristics. Here are the key differences:
- Underlying cause: Kwashiorkor is primarily caused by a deficiency of dietary protein, even when the overall caloric intake may be sufficient. On the other hand, Marasmus is caused by a severe deficiency of both calories and protein. [7] [8]
- Physical appearance: Children with Kwashiorkor often exhibit edema, which is the swelling of the body due to fluid retention. This edema is most commonly seen in the legs, feet, and face. In contrast, children with Marasmus have a wasting appearance, characterized by severe weight loss, muscle wasting, and a generally emaciated appearance. [7] [8]
- Body composition: Kwashiorkor is associated with an imbalance in body composition, where there is an accumulation of fat in the liver and other organs, despite overall muscle wasting. In Marasmus, there is a generalized loss of body fat and muscle mass. [7] [8]
- Clinical symptoms: Kwashiorkor is typically associated with dermatological changes such as skin lesions, hair changes (e.g., discolouration or thinning), and a flaky rash known as desquamation. In contrast, Marasmus is characterized by extreme weight loss, growth retardation, extreme weakness, and a weakened immune system. [7] [8]
- Age of onset: Kwashiorkor commonly affects children between 1 and 3 years old, while Marasmus is more prevalent in infants under one year of age.
It’s important to note that Kwashiorkor and Marasmus can coexist or transition from one form to another, especially in severe cases. Proper diagnosis and treatment are crucial to addressing these conditions effectively. If you need more information or have further questions, feel free to ask!
FAQs
What does Ayurveda recommend for treating diseases like Kwashiorkor and Marasmus?
Ayurveda emphasizes a balanced diet that includes all essential nutrients. A diet rich in fresh fruits, vegetables, whole grains, and dairy products like milk can support overall health. Additionally breastfeeding children for at least 6 months after they are born is recommended to prevent the onset of Marasmus.
Are Kwashiorkor and Marasmus only found in developing countries?
While Kwashiorkor and Marasmus are more prevalent in developing countries with limited access to nutritious food, they can also occur in other regions, particularly in vulnerable populations or during periods of famine or crisis.
Are there any long-term effects of Kwashiorkor and Marasmus?
Both Kwashiorkor and Marasmus can have long-lasting effects on physical and cognitive development if not treated promptly. Stunted growth, impaired brain development, weakened immune system, and increased susceptibility to infections are some of the potential long-term consequences.
Can Kwashiorkor and Marasmus be diagnosed through specific tests?
There isn’t a single test specifically for diagnosing Kwashiorkor or Marasmus. Diagnosis is typically based on a combination of physical examination, medical history, and assessment of the child’s nutritional status. Blood tests may be conducted to evaluate levels of certain nutrients or to identify any underlying infections or complications.
Are Kwashiorkor and Marasmus reversible conditions?
With proper and timely treatment, both Kwashiorkor and Marasmus can be reversed. Nutritional rehabilitation, along with medical interventions to address underlying infections or complications, can help restore the child’s health and promote normal growth and development.
Conclusion
In summary, while both Kwashiorkor and Marasmus are forms of severe malnutrition, they differ in their causes, symptoms, and management approaches. Kwashiorkor is primarily caused by a lack of protein intake, while Marasmus results from deficiencies in both calories and protein. Understanding these differences is crucial for effective management and prevention of these conditions. Addressing malnutrition requires a comprehensive approach that includes proper nutritional rehabilitation, medical intervention, and ongoing support for both the affected individual and their caregivers.
Disclaimer: This Article is for informative purposes only and does not constitute medical advice. Kindly contact a medical professional before attempting any treatments mentioned in the article yourself.
References:
- Understanding PEM In Ayurveda With Management (iamj.in)
- Listening to the Ga: Cicely Williams’ Discovery of Kwashiorkor on the Gold Coast (wphna.org)
- Kwashiorkor: still an enigma – the search must go on (ennonline.net)
- Kwashiorkor – an overview | ScienceDirect Topics
- Mechanisms of Kwashiorkor-Associated Immune Suppression: Insights From Human, Mouse, and Pig Studies (frontiersin.org)
- Difference between kwashiorkor and marasmus: Comparative meta-analysis of pathogenic characteristics and implications for treatment – PubMed (nih.gov)
- Malnutrition in Sub – Saharan Africa: burden, causes and prospects – PMC (nih.gov)
- Marasmus (europepmc.org)
- Health complication caused by protein deficiency. (researchgate.net)
- Malnutrition in Sub – Saharan Africa: burden, causes and prospects | Pan African Medical Journal (ajol.info)